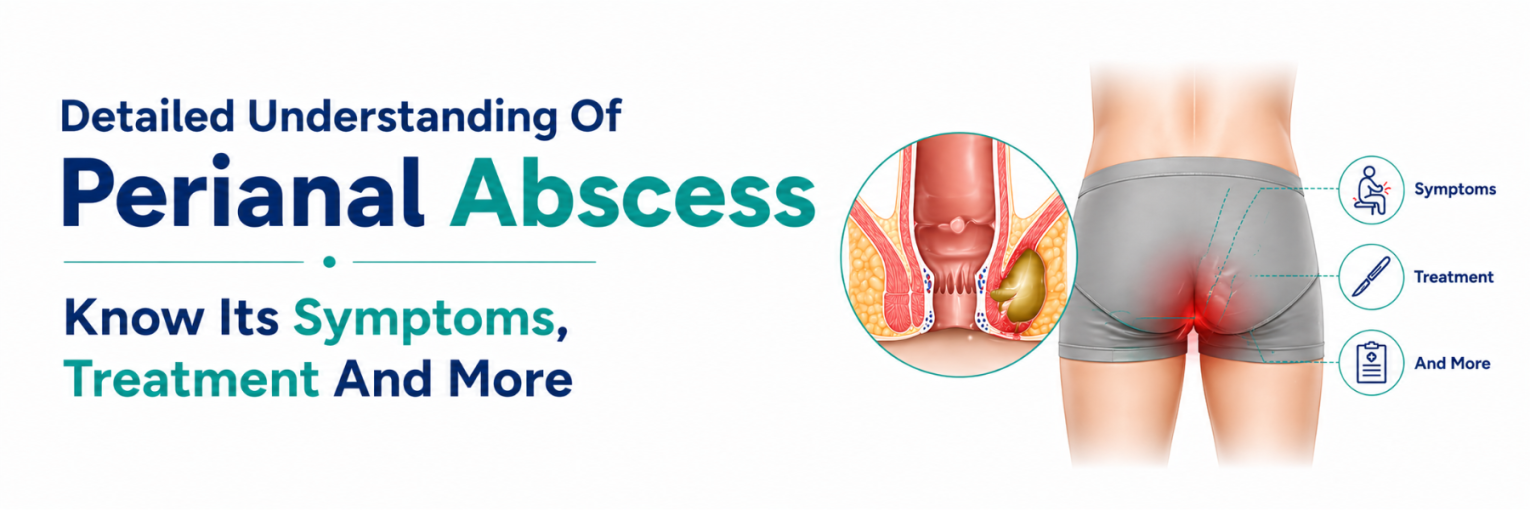
A perianal abscess is a painful infection near the anus where in pus collects under the skin or in deeper tissues. It usually starts when a small gland in the anal canal becomes blocked and infected. Many patients first notice increasing pain and a tender swelling, followed by other conditions. This blog explains perianal abscess symptoms, how doctors confirm the diagnosis, and when perianal abscess surgery is advised.
What is a Perianal Abscess?
A perianal abscess is a localised pocket of pus that forms close to the anus, the lower rectum, or the surrounding perineal skin. It often appears as a swollen, tender lump and may be associated with redness and warmth of the nearby skin. The pain can be significant because the area has many nerve endings and is involved in sitting and bowel movements.
- The anal canal contains several small glands that release mucus and support normal bowel function. When the opening of one of these glands becomes blocked, bacteria can become trapped inside. The body responds with inflammation, and pus begins to collect. This process is the most common explanation for a perianal abscess infection.
- It is also important to understand how an abscess differs from a fistula. An abscess is an active infection with pus in a cavity. A fistula is an abnormal channel that may form between the anal canal and the skin after an abscess, or it may develop alongside it. When a fistula is present, the risk of recurrence is higher, and treatment planning changes.
Symptoms of Perianal Abscess
Perianal abscess symptoms usually develop over a short period. The most frequent complaint is pain near the anus that becomes progressively worse. Many patients describe discomfort while sitting, during bowel movements, and sometimes even at rest.
Common perianal abscess symptoms include:
| Symptom | What to monitor |
| Pain near the anus (progressively worse) | Pain develops over a short period and often increases steadily. |
| Discomfort with sitting or bowel movements | Pain may worsen while sitting and during bowel movements |
| Tender swelling or lump near the anus | A painful, tender swelling or lump close to the anal opening. |
| Redness and warmth | Surrounding skin may look red and feel warm due to inflammation. |
| Persistent throbbing pain | Pain may throb and increase with movement. |
Not every patient develops a fever. A deeper abscess can cause severe pain even when the skin looks relatively normal. For that reason, ongoing intense pain with or without visible swelling should be assessed clinically.
Many people search for lumpy swelling conditions in this area because piles, fissures, skin boils, and abscesses can appear similar at first. A targeted evaluation helps avoid delays and reduces the risk of complications.
Causes of Perianal Abscess
The recognised perianal abscess causes include:
- Infection related to an anal fissure (a tear in the anal lining)
- Local trauma that allows bacteria to enter the tissues around the anus
- Certain sexually transmitted infections, depending on exposure and clinical findings
- Inflammatory bowel disease, which increases the risk of perianal infection and fistula formation
- Diabetes can increase infection risk and affect healing when blood sugar is not well controlled
- Reduced immunity due to immunosuppression medicines or medical conditions, which can lead to more severe infections
- Infection of a nearby cyst, such as an epidermoid (sebaceous) cyst, which can sometimes mimic an abscess
- Hidradenitis suppurativa affecting the groin or perianal area, which can cause repeated nodules, draining sinuses, and abscess-like lesions
When clinicians evaluate recurrent perianal abscess causes, they often focus on whether a fistula is present. A fistula can continue to seed infection, leading to repeated abscess formation. Other contributors to recurrence include poorly controlled diabetes and smoking.
A patient may also ask whether a perianal abscess is contagious. The infection itself is local and usually originates from bacteria that are already present in the bowel and skin environment. The concern is not casual spread to others, but progression of infection within the affected individual if treatment is delayed.
Diagnosis in a Clinical Setting
Diagnosis is usually based on history and a careful examination. The clinician typically asks about pain pattern, fever, discharge, bowel habits, prior similar episodes, diabetes, immune status, and any history of inflammatory bowel disease. These details help estimate whether the abscess is superficial or deep and whether additional testing is needed.
- A physical examination may include inspection of the perianal skin to look for swelling, redness, drainage points, or tenderness.
- In some cases, pain limits examination, and imaging is used to confirm the location before a procedure.
Treatment for Perianal Abscess
Perianal abscess treatment is chosen based on abscess size, depth, pain severity, fever, and patient risk factors. In many cases, the definitive treatment is drainage because antibiotics alone often cannot penetrate a sealed pus cavity effectively.
Patients should not attempt home drainage. Attempting to puncture or squeeze the area can worsen tissue injury, increase bacterial spread, and delay appropriate care.
Drainage as the Main Treatment
- For many patients, drainage is a minor procedure performed under local anaesthesia in a clinic, especially when the abscess is superficial and clearly localised. The clinician makes a small incision to release pus and reduce pressure. Pain often improves soon after effective drainage.
- When the abscess is large, deep, or associated with significant fever, drainage may be done in a hospital setting. In such situations, anaesthesia may be used to allow a complete and safe procedure. This scenario is often described by patients as perianal abscess surgery, even though the main aim is drainage rather than removal of tissue.
- If the cavity is extensive or continues to drain, the clinician may place a small drain to allow ongoing drainage for a short period. Dressings are commonly used, and the wound is allowed to heal gradually from the inside outward.
Use of Antibiotics
Antibiotics may be recommended in selected situations rather than for every abscess. A clinician may prescribe antibiotics when any of the following are present:
- Fever, chills, or other signs of systemic infection
- Spreading skin infection around the abscess
- Diabetes, immuno suppression, or other risk factors for complicated infection
- Concern about deeper infection based on examination or imaging findings
Even when antibiotics are prescribed, drainage may still be required if pus collection is confirmed.
After-Procedure Care and Comfort Measures
- After drainage, doctors often advise steps that reduce pain and support healing. These may include warm sitz baths, careful hygiene, and regular dressing changes as instructed.
- Patients are usually advised to return for follow-up if pain does not improve, fever continues, discharge remains heavy, or swelling reappears. These features can indicate incomplete drainage, a deeper pocket, or fistula development.
Perianal Abscess Treatment Guidelines and Follow-Up Planning
Perianal abscess treatment guidelines used in colorectal practice generally prioritise prompt drainage for confirmed abscesses. Follow-up is important because a proportion of patients may develop a fistula after an abscess episode. This is not always preventable, but early recognition improves planning and reduces repeated infections.
If there is persistent drainage, recurrent swelling, or repeated infections, the treating doctor may recommend further evaluation to look for a fistula tract or for underlying bowel disease. This is one of the reasons diagnostic centres play a valuable role in follow-up imaging and reporting.
Perianal Abscess Treatment Without Surgery
- Patients often ask about perianal abscess treatment without surgery. If there is no clear pus cavity and symptoms are mild, a clinician may advise close observation with local care such as warm sitz baths, warm compresses, and pain control, with strict return precautions. This approach may be considered for very small early lesions where an abscess has not fully formed.
- However, once a true abscess cavity is present, drainage is frequently required for resolution. If the abscess opens and drains on its own, clinical assessment is still recommended. Spontaneous drainage does not confirm that the cavity has fully emptied, and it does not rule out a fistula.
- Recovery time depends on abscess size, depth, and whether there are additional issues such as diabetes or immuno suppression. Many patients notice meaningful pain relief soon after drainage, while complete healing can take several weeks. The treating clinician provides individual guidance based on the wound and symptom course.
Imaging Requirement for Perianal Abscess
Many superficial abscesses can be diagnosed on examination and treated without imaging. Imaging is needed in cases where the abscess location is uncertain or the infection is suspected to be deep. This approach avoids unnecessary tests and ensures that complex diseases are not missed.
Imaging is commonly considered in these situations:
- Severe perianal or rectal pain with minimal visible swelling
- Suspected deep abscess based on tenderness pattern or systemic symptoms
- Persistent discharge after treatment, which can suggest a fistula
- Suspected multiple pockets, where a single incision may not drain the entire infection
- Immunocompromised patients, where infections may progress rapidly or present atypically
- Known or suspected Crohn’s disease, where fistula and deep sepsis are more common
- Failure to improve after drainage and initial treatment
Ultrasound
Ultrasound can help detect a fluid collection close to the skin surface and can sometimes guide localisation. Some centres use specialised approaches for perianal assessment. Ultrasound is typically more useful for superficial collections and may be less informative for complex fistula mapping than MRI.
MRI Pelvis
MRI is often the preferred test when a fistula is suspected or when the abscess is deep. It provides high-detail images of soft tissue planes and can show the relationship of infection to the anal sphincters. This detail helps clinicians plan appropriate treatment and reduces the risk of missed fistulous tracts.
MRI is also helpful when symptoms suggest a problem, but examination does not clearly show a superficial abscess. In such cases, MRI can confirm whether an abscess is present and clarify its extent.
CT Scan
CT is sometimes used when there is concern for extensive infection spread, pelvic involvement, or urgent evaluation when MRI is not feasible. CT may also be selected in emergency settings when rapid imaging is required.
A diagnostic centre will usually require a clinician’s referral for imaging, and the centre will provide preparation instructions. For MRI, standard safety screening is important, especially for implanted devices or a metal exposure history.
FAQs
What are the first warning signs of a perianal abscess?
Early signs often include increasing pain near the anus, a tender swelling, redness, and discomfort while sitting or during bowel movements. Some patients develop a fever. Any rapidly worsening pain or swelling should be assessed promptly.
Can a perianal abscess go away on its own with antibiotics?
A true abscess often needs drainage because antibiotics may not reach the pus cavity effectively. Antibiotics may be added in selected cases, but they are not a reliable substitute for drainage when a collection of pus is present.
How does a doctor tell the difference between an abscess and a fistula?
An abscess usually causes acute pain and swelling, while a fistula often causes persistent or recurrent discharge and repeated infections. Examination can suggest the difference. Imaging such as MRI may be needed to confirm a fistula and map its path.
Why would I need an MRI or ultrasound for a simple abscess?
It is recommended when the abscess is suspected to be deep and when findings are unclear. It is needed when symptoms recur. Imaging helps locate the infection accurately and supports treatment planning.
Is a perianal abscess considered a medical emergency?
It can become urgent, especially if there is fever, severe or rapidly increasing pain, spreading redness, or signs of systemic infection. People with diabetes or reduced immunity should seek assessment early because complications can develop faster.
What is the standard procedure for draining a perianal abscess?
The standard approach is incision and drainage performed by a trained clinician. Small superficial abscesses may be drained under local anaesthesia, while deep or complex cases may require drainage in an operating theatre under anaesthesia.
What are the risks of leaving a perianal abscess untreated?
Without treatment, the infection may enlarge, spread to deeper tissues, and cause more severe illness. Delayed care can also increase the chance of fistula formation and may lead to more extensive procedures and a longer recovery period.